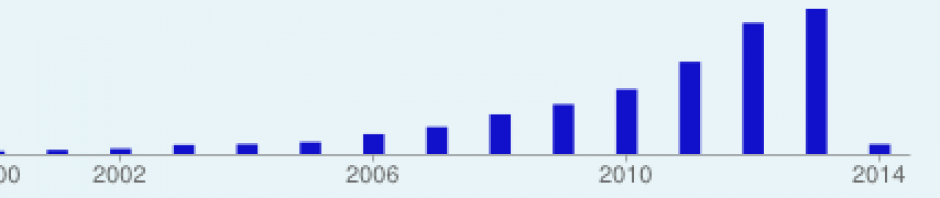
In an earlier post, I presented estimates of drug overdose deaths in 2019 for the world and selected countries. The USA accounted for an astonishing 40% of global drug overdose deaths and an even higher percentage of global opioid overdose deaths.
More recently, it has been estimated that deaths from drug overdose rose by an estimated 13% in the first half of 2020 compared to 2019 [1]. In some states, drug related deaths climbed by over 30%. Its unclear whether the increasing social isolation, pressure on health services, and lockdowns associated with the pandemic, particularly in the second half of 2020, will result in continued increase [2].
I’ve updated the previous estimates for years 2000-2019 to take into account revised inputs from the 2019 Global Burden of Disease [3] used for projecting trends to 2019 from an earlier update to 2017 (see previous post). The revised estimates are slightly higher than those presented in the previous post:

Assuming a somewhat more conservative 10% increase for 2020 than observed in the first half of the year, there were a little over 80,000 drug overdose deaths in the USA in 2020, of which the majority (close to 60,000) would have been opioids. Initially driven by prescription opioid painkillers in earlier years, users migrated first to heroin and then to fentanyl, which is cheaper (much of it illicitly made). The global average death rate for drug use disorders was 24 per million population, compared with 225 per million for the USA. In other words, the USA rate is 9 times higher than the global average.
Trends in drug use disorder deaths by WHO Region
The following regional graphs highlight how different the situation in the USA is to the rest of the world (grouped in the World Health Organization regions).

Drug overdose death rates per million population, for USA and WHO Regions, 2000-2019
The analysis of death registration data is complicated by the need to distribute the accidental poisoning category for “other and unspecified chemicals and noxious substances” (X49) to the specific categories for alcohol and drug use disorders (opioids, cocaine, amphetamines, cannabis and “other drugs”) and to accidental poisoning (non-drug and non-alcohol). Additionally, there is a category F19 in the mental health chapter for “multiple drug use and unspecified drug use disorders” which is used to code deaths in some countries and also must be redistributed appropriately. So there is some uncertainty associated with the estimates for countries with death registration data, and even more for countries without good data.
Total attributable drug deaths
A little over 10 years ago, I carried out an updated comparative risk assessment of the total deaths and burden of disease associated with various risk factor exposures, including drug use (licit and illicit) [4]. More recently, drawing on reviews and analyses carried out by expert groups advising WHO and IHME on drug and alcohol use, I updated the drug use estimates for the year 2017 to include the excess deaths from infectious diseases associated with injecting drug use, as well as road injury and suicide. These analyses were carried out using comparative risk assessment methods [5].
I’ve projected these analyses forward to 2019 using the updated cause of death estimates to 2019 and assuming previously calculated population attributable fractions for 2017 remain constant to 2019. These will provide ballpark estimates at global level that will give a reasonably good picture of the comparative contributions of the main drug types and the main disease and injury outcomes to the total mortality attributable to drug use.
Before giving a little more detail on data and methods used, I will present a summary of the overall results for 2019 at global level.

For the calculation of the fraction of cause-specific deaths attributable to drug use, country-specific time series of prevalences of drug dependence were taken from the Global Burden of Disease [6] based on estimates prepared by an expert group [7].
Road injury and suicide
Relative risks for deaths from road injury by drug type were based on results of a systematic review by Elvik (8). This evidence is discussed in more detail in a later WHO publication (9). Based on advice from a WHO Technical Advisory Group (10), the relative risk for road injury death associated with drug use was based on studies reported by Elvik (8) which controlled for at least three of the main confounding factors.
Relative risks for suicide were derived from a systematic review and meta-analysis (11). The evidence for association of suicide with cannabis use was considered not strong enough. Insufficient information was available to quantify any risk of psychosis associated with cannabis use.
Attributable fractions for injecting drug use (IDU)
Relative risks for deaths due to HIV, HBV and HCV infection due to injecting drug use have been estimated by Degenhardt et al based on available studies (12, 13).Degenhardt et al (14, 15) estimated the fractions of deaths due to HIV, HBV and HCV (and the liver cancer and cirrhosis attributed to HBV and HCV) by country for year 2013. These were used in GBD2017 to estimate population attributable fractions (PAFs) for these causes by country, year, age and sex. These PAFs are then applied to my provisional cause of death estimates for years 2000-2019 to estimate attributable deaths for IDU. These deaths are apportioned to the specific drug types using an informal review of literature carried out by WHO colleagues for the 2017 update [16]. The drug type distribution is assumed to hold constant across years 2000-2019.
Previous updates of attributable deaths for drug use have included estimates of uncertainty, combining uncertainty in cause of death estimates [17] with uncertainty in drug use prevalences and relative risks. I haven’t updated these uncertainty intervals for this update, which provides a broad picture of the current relative health impacts of the main types of drug use. It should be remembered that these drug categories include licit and illicit use.

Alcohol, tobacco and drugs
The following table and figure summarizes and compares the estimated global deaths attributable to tobacco, alcohol and drugs in 2019. Tobacco causes by far the largest death toll, almost 9 million deaths representing almost 15% of all deaths globally in 2019. Following is alcohol, responsible for around 5% and then drugs causing just under 1% of global deaths. For comparison, there were 1.83 million recorded deaths from Covid-19 in 2020, though actual total deaths were undoubtedly higher (perhaps as many as 2.7 to 3.6 million).
The attributable burden of disease, in terms of DALYs which measure equivalent lost healthy years of life from both poor health and premature mortality, gives relatively higher weight to alcohol. While I’ve not updated DALY estimates to 2019, the GBD 2019 [3] estimates global attributable DALYs for 2019 as 230 million for tobacco, 93 million for alcohol, and 31 million for drug use. Unlike tobacco which kills most people at older ages with relatively limited periods of disability, alcohol and drug use are associated with significant loss of health at younger ages, and drug deaths in particular tend to occur at younger adult ages rather than older ages. The estimates for alcohol and drugs are somewhat higher than those of the GBD 2019, at 2.4 million for alcohol and 494 thousand for drugs [3].

The attributable burden of disease, in terms of DALYs which measure equivalent lost healthy years of life from both poor health and premature mortality, gives relatively higher weight to alcohol. While I’ve not updated DALY estimates to 2019, the GBD 2019 [3] estimates global attributable DALYs for 2019 as 230 million for tobacco, 93 million for alcohol, and 31 million for drug use. Unlike tobacco which kills most people at older ages with relatively limited periods of disability, alcohol and drug use are associated with significant loss of health at younger ages, and drug deaths in particular tend to occur at younger adult ages rather than older ages.
Acknowledgements
Previous estimates of deaths attributable to drug use prepared for WHO for 2017 and earlier years benefited from substantial advice and inputs from WHO expert advisors and staff, particularly Juergen Rehm, Louisa Degenhardt and Vladimir Pozniak. The estimates presented here are my ballpark estimates based on quick update and do not represent the views of WHO or anyone else.
References
[1] Wen LS, Sadeghi NB. The opioid crisis and the 2020 US election: crossroads for a national epidemic. The Lancet Volume 396, ISSUE 10259, P1316-1318, October 24, 2020. DOI:https://doi.org/10.1016/S0140-6736(20)32113-9
[2] Katz J, Goodnough A, Sanger-Katz M. In Shadow of Pandemic, U.S. Drug Overdose Deaths Resurge to Record. New York Times, July 15, 2020. Available from https://www.nytimes.com/interactive/2020/07/15/upshot/drug-overdose-deaths.html
[3] Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2019 (GBD 2019) Results. Seattle, United States: Institute for Health Metrics and Evaluation (IHME), 2020. Available from http://ghdx.healthdata.org/gbd-results-tool.
[4] Mathers CD, Stevens G, Mascarenhas M. Global health risks: mortality and burden of disease attributable to selected major risks. WHO, Geneva, 2009.
[5] Ezzati M, Lopez AD, Rodgers A, Vander Hoorn S, Murray CJL. Comparative quantification of health risks: global and regional burden of disease attributable to selected major risk factors. Geneva: World Health Organization. 2004
[6] Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2017 (GBD 2017) Results. Seattle, United States: Institute for Health Metrics and Evaluation (IHME), 2018.
[7] Peacock A., Hall W., Degenhardt L. (2019) Epidemiology of Substance Use Internationally. In: Sloboda Z., Petras H., Robertson E., Hingson R. (eds) Prevention of Substance Use. Advances in Prevention Science. Springer, Cham. https://doi.org/10.1007/978-3-030-00627-3_2.
[8] Elvik, R (2013). Risk of road accident associated with the use of drugs: a systematic review and meta-analysis of evidence from epidemiological studies. Accid Anal Prev. 2013 Nov;60:254-67. doi: 10.1016/j.aap.2012.06.017. Epub 2012 Jul 9.
[9] World Health Organization (2016). The health and social effects of nonmedical cannabis use. Geneva: WHO. Available at https://www.who.int/substance_abuse/publications/msb_cannabis_report.pdf
[10] World Health Organization (2015). Technical Advisory Group on Alcohol and Drug Epidemiology Meeting (unpublished report). Geneva: WHO, November 2015.
[11] Ferrari AJ, Norman RE, Freedman G, Baxter AJ, Pirkis JE, Harris MG, Page A, Carnahan E, Degenhardt L, Vos T, Whiteford HA (2014). The burden attributable to mental and substance use disorders as risk factors for suicide: findings from the Global Burden of Disease Study 2010. PLoS One. 2014 Apr 2;9(4):e91936. doi: 10.1371/journal.pone.0091936. eCollection 2014.
[12] Degenhardt, L, Whiteford HA, Ferrari AJ, Baxter AJ, Charlson WD, Hall WD, et al. (2013). Global burden of disease attributable to illicit drug use and dependence: findings from the Global Burden of Disease Study 2010. Lancet 382 (9904): pp. 1564– 74.
[13] Van Den Berg C, Smit C, Van Brussel G, Coutinho R, Prins M; Amsterdam Cohort (2007). Full participation in harm reduction programmes is associated with decreased risk for humanimmunodeficiency virus and hepatitis C virus: evidence from the Amsterdam Cohort Studies among drug users. Addiction. 2007 Sep;102(9):1454-62.
]14] Degenhardt et al (2016). Estimating the burden of disease attributable to injecting drug use as a risk factor for HIV, hepatitis C, and hepatitis B: findings from the Global Burden of Disease Study 2013. Lancet Infectious Diseases 2016, 16:1385-98.
[15] Degenhardt et al (2017). Global prevalence of injecting drug use and sociodemographic characteristics and prevalence of HIV, HBV, and HCV in people who inject drugs: a multistage systematic review. The Lancet Global Health 2017; 5:31192-207.
[16] Poznyak V, et al. (2016). Unpublished review of the distribution of injecting drug use by type. World Health Organization.
[17] World Health Organization (2018). WHO methods and data sources for global burden of disease estimates 2000-2016 (Global Health Estimates Technical Paper WHO/HIS/IER/GHE/2018.4)
[18] World Health Organization (2018). Global Status Report on Alcohol and Health 2018. WHO: Geneva. https://www.who.int/publications/i/item/9789241565639